- Home
- Cancer of the uterus
- About cancer of the uterus
About cancer of the uterus
Cancer of the uterus (also called uterine cancer or endometrial cancer) occurs when cells in any part of the uterus become abnormal, grow out of control and form a lump (tumour).
Learn more about:
For your community
Types of cancer of the uterus
Cancer of the uterus can be either endometrial cancer (which accounts for about 95% of cancers of the uterus) or the less common uterine sarcoma (which accounts for about 5%).
Endometrial cancers
This cancer begins in the cells in the lining of the uterus (called the endometrium). Endometrial cancer is divided into 4 main subtypes. Knowing these subtypes helps the doctor to work out what, if any, treatment is needed after surgery. Tests on tissue samples collected before or during surgery help the doctor to work out the subtype.
The 4 subtypes are:
- POLE mutant – usually treated with surgery only; often has a good outcome
- mismatch repair deficient (MMRd) – additional treatment like immunotherapy may be needed after surgery; may be inherited (Lynch syndrome)
- p53 abnormal – usually needs treatment after surgery
- no specific molecular profile (NSMP) – may need treatment after surgery.
Uterine sarcomas
These rare soft tissue cancers develop in the cells in the muscle of the uterus (myometrium) or connective tissue (stroma). There are 3 types:
- endometrial stromal
- leiomyosarcoma
- undifferentiated.
Much of our information about cancer of the uterus will be relevant if you have uterine sarcoma. You can also read more about this type of cancer at Soft Tissue Sarcoma.
Who gets cancer of the uterus?
Each year, about 3400 Australian women are diagnosed with cancer of the uterus, and most are over 50 years of age. Cancer of the uterus is the fifth most common cancer in women and the most commonly diagnosed gynaecological cancer (cancer affecting the female reproductive system).
The number of women diagnosed with cancer of the uterus has increased in recent years, including in younger women. This is likely to be linked to rising rates of obesity and diabetes, as well as more people living to older ages.
Anyone with a uterus can get cancer of the uterus – women, transgender men, non-binary people and people with intersex variations. For information specific to you, speak to your doctor. For more on this, see LGBTQI+ People and Cancer.
What causes cancer of the uterus?
The exact cause of cancer of the uterus is unknown, but factors that can increase the risk include:
- age – cancer of the uterus is most common in women aged over 50 and in women who have stopped having periods (postmenopausal)
- body weight – carrying extra body weight (overweight or obese) is a major risk factor
- medical factors – having diabetes; having previous radiation therapy for cancer in the pelvic area; having endometrial hyperplasia
- family history – having one or more close blood relatives diagnosed with uterine, ovarian or bowel cancer; or inheriting a genetic condition such as Lynch syndrome or Cowden syndrome
- reproductive history – not having children
- hormonal factors – starting periods before the age of 12; going through menopause after the age of 55; taking some types of oestrogen-only menopausal hormone therapy (MHT, previously called hormone replacement therapy or HRT); or taking tamoxifen, an anti-oestrogen drug used for breast cancer.
Many people who have risk factors don’t develop cancer of the uterus, and some people who get this cancer have no risk factors. If you are concerned about any risk factors, talk to your doctor. Maintaining a healthy body weight and being physically active are the best ways to reduce the risk of developing cancer of the uterus.
For an overview of what to expect at every stage of your cancer care, visit Cancer Care Guides – Endometrial cancer. This is a short guide to what is recommended for endometrial cancer, from diagnosis to treatment and beyond.
Other conditions of the uterus
Some conditions can affect the uterus and cause abnormal vaginal bleeding and pain. They may be found during tests for cancer of the uterus.
| Polyps | Small, soft growths attached to the inner wall of the uterus. Polyps are usually benign (not cancer), but some may turn into cancer. They can be removed during a hysteroscopy and tested for cancer. |
| Fibroids | Benign tumours that begin in the muscle layer of the uterus (myometrium). Surgery may be used to reduce the size of the fibroid (myomectomy) or remove the uterus (hysterectomy). |
| Endometrial hyperplasia | Thickening of the uterus lining (endometrium) caused by too much oestrogen. Usually benign, but can lead to cancer, so may be treated with hormones, minor surgery or, in some cases, hysterectomy. |
| Endometriosis | When endometrial tissue grows outside the uterus (e.g. in the abdomen). Does not usually lead to cancer. May be treated with surgery or hormones. |
The uterus
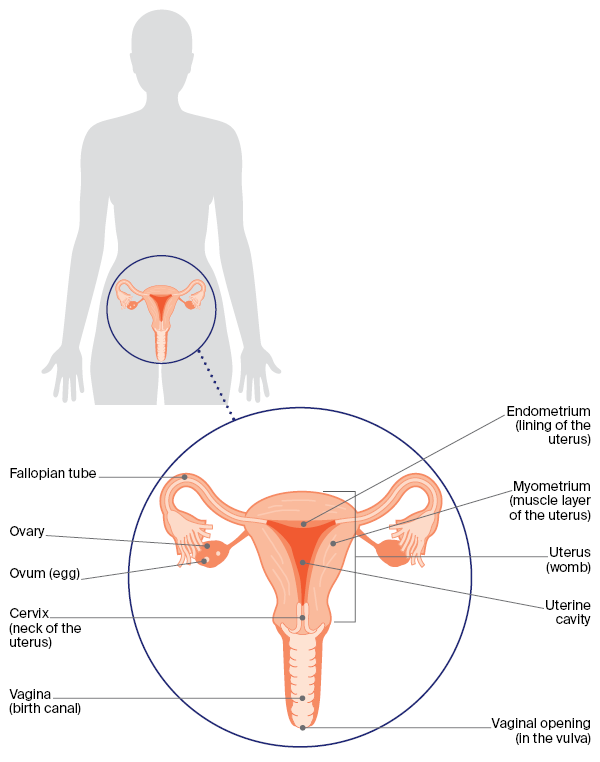
The uterus, or womb, is where a baby grows during pregnancy. It is part of the female reproductive system, which also includes the ovaries, fallopian tubes, cervix (neck of the uterus), vagina (birth canal) and vulva (external genitals).
The shape and position in the body
The uterus is about the size and shape of a hollow, upside-down pear. It sits low in the abdomen (belly) between the bladder and rectum, and is joined to the vagina by the cervix. The ovaries sit on either side of the uterus. The ovaries contain eggs (ova) and are connected to the uterus by the fallopian tubes.
The layers of the uterus
The uterus has 2 layers. The myometrium is the outer layer of muscle tissue and makes up most of the uterus. The endometrium is the inner layer or lining.
The female reproductive system
Menstruation
Each month, from puberty to menopause, the endometrium becomes thicker to prepare for pregnancy. If a pregnancy does not occur, some of the lining is shed and flows out of the body through the vagina. The flow is called a monthly period or menstruation.
Menopause
The hormones oestrogen and progesterone control the release of eggs (ovulation) and the timing of menstruation. As you get older, the ovaries gradually produce less of these hormones. When the levels of oestrogen and progesterone fall low enough, periods become irregular and finally stop. This is known as menopause. After menopause, it is not possible to conceive a child naturally. The uterus also becomes smaller and the endometrium becomes thinner.
→ READ MORE: Cancer of the uterus symptoms
More resources
All updated content has been clinically reviewed by Professor Alison Brand, Clinical Professor, The University of Sydney and Director, Department of Gynaecological Oncology, Westmead Hospital, NSW. This edition is based on the previous edition, which was reviewed by the following panel: A/Prof Orla McNally, Consultant Gynaecological Oncologist, Director Oncology/Dysplasia, Royal Women’s Hospital, Honorary Clinical Associate Professor, University of Melbourne, and Director of Gynaecology Tumour Stream, Victorian Comprehensive Cancer Centre, VIC; A/Prof Yoland Antill, Medical Oncologist, Peninsula Health, Parkville Familial Cancer Centre, Cabrini Health and Monash University, VIC; Grace Guerzoni, Consumer; Zeina Hayes, 13 11 20 Consultant, Cancer Council Victoria; Bronwyn Jennings, Gynaecology Oncology Clinical Nurse Consultant, Mater Hospital Brisbane, QLD; A/Prof Christopher Milross, Director of Mission and Radiation Oncologist, Chris O’Brien Lifehouse, NSW; Mariad O’Gorman, Clinical Psychologist, Liverpool Cancer Therapy Centre and Bankstown Cancer Centre, NSW.
View the Cancer Council NSW editorial policy.
View all publications or call 13 11 20 for free printed copies.

