- Home
- Bowel cancer
- About bowel cancer
About bowel cancer
Bowel cancer is cancer in any part of the large bowel (colon or rectum). It is sometimes known as colorectal cancer and might also be called colon cancer or rectal cancer, depending on where in the bowel it is found.
Learn more about:
What is bowel cancer?
This is cancer that starts in the inner lining of the bowel wall. It usually develops from small growths called polyps. Most polyps are harmless (benign), but some may turn into cancer. To prevent this, polyps can be removed during a colonoscopy.
If untreated, bowel cancer can grow into the deeper layers of the bowel wall. It can spread from there to the lymph nodes and nearby organs such as the prostate or bladder. If the cancer advances further, it can spread to other organs, such as the liver or lungs.
The bowel
The bowel is part of the lower gastrointestinal (GI) tract, which is part of the digestive system. The digestive system starts at the mouth and ends at the anus. It helps the body break down food and turn it into energy. It also gets rid of the parts of food the body does not use.
The small bowel (small intestine)
This is a long tube (4–6 m) that absorbs nutrients from food. The small bowel is longer and narrower than the large bowel. It has 3 parts:
- duodenum – the top section; receives broken-down food from the stomach
- jejunum – the middle section
- ileum – the lower and longest section; moves waste into the large bowel.
The large bowel (large intestine)
This tube is about 1.5 m long. It absorbs water and salts, and turns what is left into solid waste (known as faeces, stools or poo when it leaves the body). The large bowel has 3 parts:
- caecum – looks like a pouch; it receives waste from the small bowel
- colon – the main working area of the large bowel, the colon makes up most of the large bowel’s length and has 4 parts (ascending colon, transverse colon, descending colon and sigmoid colon); the term colon is often used to refer to all 4 parts of the colon and the caecum
- rectum – the last 15–20 cm of the large bowel.
The anus
This is the opening at the end of the large bowel. During a bowel movement, the anal muscles relax to release faeces. Cancer that affects the anus is called anal cancer.
The lower digestive system
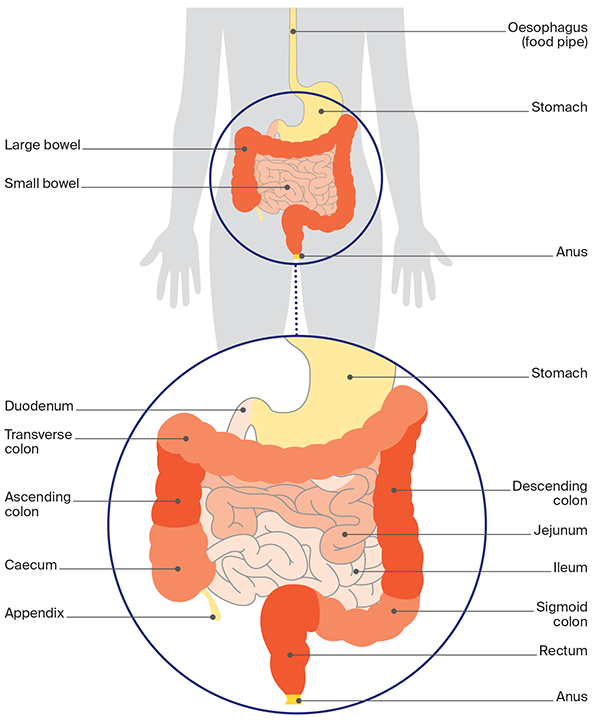
Less common types of bowel cancer
Most bowel cancers are adenocarcinomas, which start in the tissue lining the bowel. Rarely, other less common types of cancer can also affect the bowel. These include lymphomas, squamous cell carcinomas, neuroendocrine tumours and gastrointestinal stromal tumours. These types of cancer aren’t discussed in this section and treatment may be different. Call Cancer Council 13 11 20 for more information.
Cancer can also start in the small bowel (called small bowel cancer or small intestine cancer), or the appendix, but this is rare.
Who gets bowel cancer?
Bowel cancer is a very common cancer in Australia. Each year, about 15,700 Australians are diagnosed with bowel cancer. It is most common in people over 50, but it can occur at any age.
What causes bowel cancer?
The exact cause of bowel cancer is not known. Research shows that people with certain risk factors are more likely to develop bowel cancer.
Risk factors for bowel cancer include:
- older age – bowel cancer is most commonly diagnosed in people over 50, and the risk increases with age
- polyps – having a large number of polyps in the bowel
- other bowel diseases – people who have an inflammatory bowel disease, such as Crohn’s disease or ulcerative colitis, have a significantly increased risk, particularly if they have had the disease for more than 10 years
- lifestyle factors – carrying extra weight, not being physically active, having a diet high in red meat or processed meats such as salami or ham, drinking alcohol, or smoking
- strong family history – a small number of bowel cancers run in families
- other cancers – people who have had bowel cancer once are more likely to develop a second bowel cancer; some people who have had ovarian cancer or cancer of the uterus (endometrial cancer) may have an increased risk of bowel cancer
- rare genetic disorders – a small number of bowel cancers are associated with an inherited gene.
Some lifestyle habits reduce your risk of developing bowel cancer, including:
- being physically active
- maintaining a healthy weight
- cutting out processed meat
- cutting down on red meat
- drinking less or no alcohol
- not smoking
- eating wholegrains, dietary fibre and dairy foods.
Ask your doctor whether taking aspirin regularly might benefit you. Aspirin may reduce the risk of bowel cancer for some people.
Can bowel cancer run in families?
Sometimes bowel cancer runs in families. The risk of developing bowel cancer may be higher if one or more of your close family members (such as a parent, brother or sister) has had bowel cancer. The risk is higher if they were diagnosed before the age of 55, or if 2 or more close relatives on the same side of your family have had bowel cancer. A family history of some other cancers, such as cancer of the uterus (endometrial cancer), may also increase the risk.
Some people have an inherited faulty gene that increases their risk of developing bowel cancer. These faulty genes cause a small number (about 5–6%) of bowel cancers.
There are 2 main genetic conditions that occur in some families:
- Familial adenomatous polyposis (FAP) – This condition causes hundreds of polyps to form in the bowel. If these polyps are not removed, they may become cancerous.
- Lynch syndrome – This syndrome causes a fault in the gene that helps the cell’s DNA repair itself. People with Lynch syndrome have an increased risk of developing bowel cancer, cancer of the uterus, and other cancers such as kidney, bladder and ovarian.
If you are worried about your family history, talk to your doctor about having regular check-ups or ask for a referral to a family cancer clinic. To find out more, call Cancer Council 13 11 20.
For an overview of what to expect at every stage of your cancer care, visit Bowel cancer: your guide to best cancer care. This is a short guide to what is recommended, from diagnosis to treatment and beyond.
→ READ MORE: Bowel cancer symptoms
More resources
A/Prof David A Clark, Senior Colorectal Surgeon, Royal Brisbane and Women’s Hospital, QLD, The University of Queensland and The University of Sydney; Yvette Adams, Consumer; Dr Cameron Bell, Gastroenterologist, Royal North Shore Hospital, NSW; Katie Benton, Advanced Dietitian Cancer Care, Sunshine Coast University Hospital and Queensland Health, QLD; John Clements, Consumer; Dr Fiona Day, Medical Oncologist, Calvary Mater Newcastle, NSW; Alana Fitzgibbon, Clinical Nurse Consultant, GastroIntestinal Cancers, Cancer Services, Royal Hobart Hospital, TAS; Prof Alexander Heriot, Consultant Colorectal Surgeon, Director Cancer Surgery, Peter MacCallum Cancer Centre, and Director, Lower GI Tumour Stream, Victorian Comprehensive Cancer Centre, VIC; Caitriona Nienaber, 13 11 20 Consultant, Cancer Council WA; Dr Kirsten van Gysen, Radiation Oncologist, Nepean Cancer Care Centre, NSW.
View the Cancer Council NSW editorial policy.
View all publications or call 13 11 20 for free printed copies.



