- Home
- Primary bone cancer
- About primary bone cancer
About primary bone cancer
In this section we look at the different types of primary bone cancer, how common it is, and what causes it.
Learn more about:
- Overview
- The bones
- Types of primary bone cancer
- How common is it?
- What are the risk factors?
- What are the symptoms?
Overview
Bone cancer can start as a primary or secondary cancer. The 2 types are different and the information here is on primary bone cancer.
| Primary bone cancer | Means that the cancer starts in a bone. It may develop on the surface, in the outer layer or from the centre of the bone. As a tumour grows, cancer cells multiply and destroy the bone. If left untreated, primary bone cancer can spread to other parts of the body. |
| Secondary (metastatic) bone cancer | Means that the cancer started in another part of the body (e.g. breast or lung) and has spread to the bone. |
The bones
A typical healthy person has over 200 bones, which:
- support and protect internal organs
- are attached to muscles to allow movement
- contain bone marrow, which makes and stores new blood cells
- store proteins, minerals and nutrients, such as calcium.
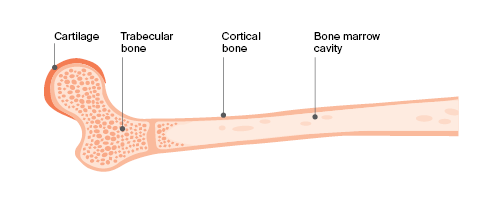
Bones are made up of different parts, including a hard outer layer (known as cortical bone) and an inner core (known as trabecular bone). The bone marrow is found in this inner core. Cartilage is the tough material at the end of each bone that allows one bone to move against another at a joint.
Bone structure
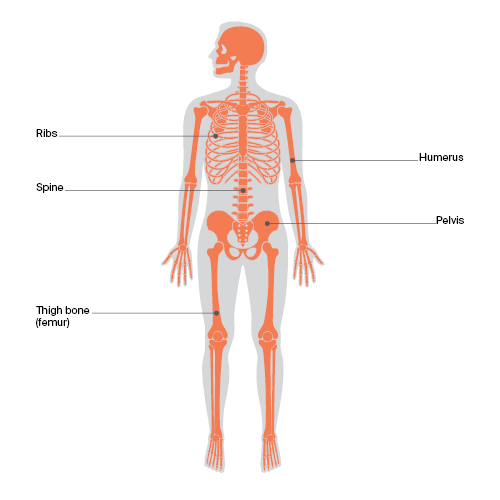
Bones of the body
Bones commonly affected by primary bone cancer include the spine, ribs, pelvis and upper bones of the arms (humerus) and legs (femur).
Types of primary bone cancer
There are more than 30 types of primary bone cancer. The most common types are:
| osteosarcoma (about 35% of bone cancers) |
|
| chondrosarcoma (about 30% of bone cancers) |
|
| Ewing sarcoma (about 15% of bone cancers) |
|
Cancer that affects the soft tissues around the bones is known as soft tissue sarcoma, and may be treated differently. For an overview of what to expect at every stage of your care for bone and soft tissue sarcomas, visit Cancer Care Guides – Sarcoma. This is a short guide to what is recommended, from diagnosis to treatment and beyond.
How common is bone cancer?
Primary bone cancer is rare. About 300 Australians are diagnosed with primary bone cancer each year.
It affects people of all ages, but most often occurs in people aged 10–25 and over 50.
What are the risk factors?
The causes of most bone cancers are unknown, but factors that may increase the risk include:
| Previous radiation exposure including radiation therapy (radiotherapy) | Radiation therapy to treat cancer increases the risk of developing bone cancer. The risk is higher when high doses of radiation therapy have been given in childhood. Most people who have radiation therapy will not develop bone cancer. |
| Chemotherapy for another cancer | Some drugs may increase the risk of osteosarcoma. |
| Other bone conditions | Some people who have Paget disease of the bone, or other benign bone conditions, are at higher risk. |
| Genetic factors | Some inherited conditions, such as Li-Fraumeni syndrome, increase the risk of bone cancer. People with a strong family history of certain types of cancer are also at risk. Ask for a referral to a family cancer clinic for more information. Some people develop bone cancer because of gene changes that happen during their lifetime, rather than inheriting a faulty gene. |
More resources
Prof Peter Choong AO, Orthopaedic Surgeon, and Sir Hugh Devine Professor, St Vincent’s Hospital, and Head of Department of Surgery, The University of Melbourne, VIC; Catherine Chapman, Adolescent and Young Adult and Sarcoma Cancer Specialist Nurse, Division of Cancer and Ambulatory Support, Canberra Hospital, ACT; A/Prof Paul Craft AM, Medical Oncologist, Canberra Hospital and Australian National University, ACT; Belinda Fowlie, Bone Tumour Nurse Practitioner Candidate, SA Bone and Soft Tissue Tumour Unit, Flinders Medical Centre, SA; Prof Angela Hong, Radiation Oncologist, Chris O’Brien Lifehouse, and Clinical Professor, The University of Sydney, NSW; Vicki Moss, Nurse Practitioner, SA Bone and Soft Tissue Tumour Unit, Flinders Medical Centre, SA; A/Prof and Dr Marianne Phillips, Paediatric and Adolescent Oncologist and Palliative Care Physician, Perth Children’s Hospital, WA; Chris Sibthorpe, 13 11 20 Consultant, Cancer Council Queensland; Stephanie Webster, Consumer.
View the Cancer Council NSW editorial policy.
View all publications or call 13 11 20 for free printed copies.