- Home
- Thyroid cancer
- Treatment
- Targeted therapy
Targeted therapy for thyroid cancer
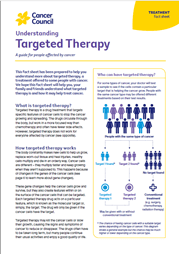
Targeted therapy drugs attack specific features of cancer cells, known as molecular targets, to stop the cancer growing and spreading.
Learn more about:
Overview
The most common targeted therapy drugs used for thyroid cancer are tyrosine kinase inhibitors (TKIs). These drugs block the chemical messengers (enzymes) that tell cancer cells to grow, multiply and spread.
If you have advanced thyroid cancer that hasn’t responded to RAI treatment, you may be offered a TKI such as lenvatinib. This drug is given as a tablet, which you take daily. You will usually keep taking the tablets for several years.
Other TKIs may be available on clinical trials, including the drug selpercatinib, which targets mutations in the RET gene. In rare or aggressive thyroid cancers, genetic tests may help your doctor tailor targeted therapy to a specific genetic mutation. Talk with your doctor about the latest developments and whether you are a suitable candidate.
Side effects of targeted therapy
The most common side effects of TKIs include:
- fatigue
- diarrhoea
- skin rash
- bleeding
- high blood pressure
In some people, TKIs can affect the way the heart and kidneys work. Some TKIs can also cause tenderness, tingling and blisters on the skin of the palms and soles. It is important to tell your doctor about any side effects immediately. If left untreated, some side effects can become life-threatening. Your doctor will explain what to watch out for, and will monitor you while you are taking targeted therapy drugs.
Video: What is targeted therapy?
Watch this short video to learn more about drug therapies, including targeted therapy and immunotherapy.
→ READ MORE: External beam radiation therapy
Podcast: Immunotherapy & Targeted Therapy
Listen now
More resources
A/Prof Diana Learoyd, Endocrinologist, GenesisCare North Shore, Faculty of Medicine and Health, University of Sydney, NSW; Emeritus Professor Leigh Delbridge AM, The University of Sydney, Thyroid Surgeon, The Mater and North Shore Private Hospitals, NSW; Prof Ruta Gupta, Tissue Pathology and Diagnostic Oncology, Royal Prince Alfred Hospital and The University of Sydney, NSW; Susan Leonard, Cancer Nurse Coordinator Thyroid and Brachytherapy, Cancer Care Services, Royal Brisbane and Women’s Hospital, QLD; Dr Dean Lisewski, Endocrine and General Surgeon, Fiona Stanley Hospital and St John of God Hospital, Murdoch, WA; Caitriona Nienaber, 13 11 20 Consultant, Cancer Council WA; Jonathan Park, Consumer; A/Prof David Pattison, Deputy Director and Senior Staff Specialist, Department of Nuclear Medicine and Specialised PET Services, Royal Brisbane and Women’s Hospital and School of Medicine, University of Queensland, QLD; Prof Bruce Robinson, Endocrinologist, Co-Head, Cancer Genetics, Kolling Institute of Medical Research, The University of Sydney and Royal North Shore Hospital, NSW; Marissa Ryan, Team Leader (Cancer) Pharmacist, Princess Alexandra Hospital, Brisbane, QLD.
View the Cancer Council NSW editorial policy.
View all publications or call 13 11 20 for free printed copies.
Need to talk?
Support services
Coping with cancer?
Ask a health professional or someone who’s been there, or find a support group or forum
Need legal and financial assistance?
Pro bono legal and financial matters, no interest loans or help with small business
Cancer information
Making cancer treatment decisions
Decision-making steps, consent and second opinions
Using targeted therapies
Information about drug therapies and immunotherapies